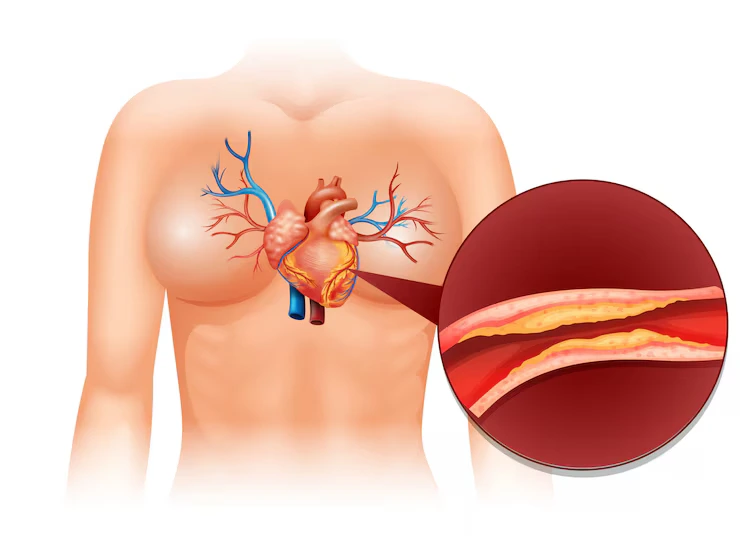
A heart attack, also known as a myocardial infarction, occurs when blood flow to part of the heart muscle is blocked for an extended period, causing damage to the heart tissue. Coronary artery disease (CAD) is the most common cause of heart attacks, where the coronary arteries that supply blood to the heart become narrowed or blocked due to plaque buildup (atherosclerosis).
Heart attacks can range from mild to life-threatening and require immediate medical attention to minimize damage to the heart and prevent further complications. Early diagnosis and treatment of CAD can help reduce the risk of heart attacks and improve outcomes.
Heart attacks and coronary artery disease are important to address because:
Dr. Gnanadev N C is a specialist in the diagnosis and treatment of heart disease, including heart attacks and coronary artery disease. With a comprehensive approach that includes lifestyle management, medications, and surgical interventions, Dr. Gnanadev provides personalized care to help prevent heart attacks, manage CAD, and improve long-term heart health. Whether for prevention, treatment, or rehabilitation, you will receive expert guidance and support for optimal cardiovascular care.
Contact us for timely diagnosis, expert guidance, and compassionate heart care.